Introduction
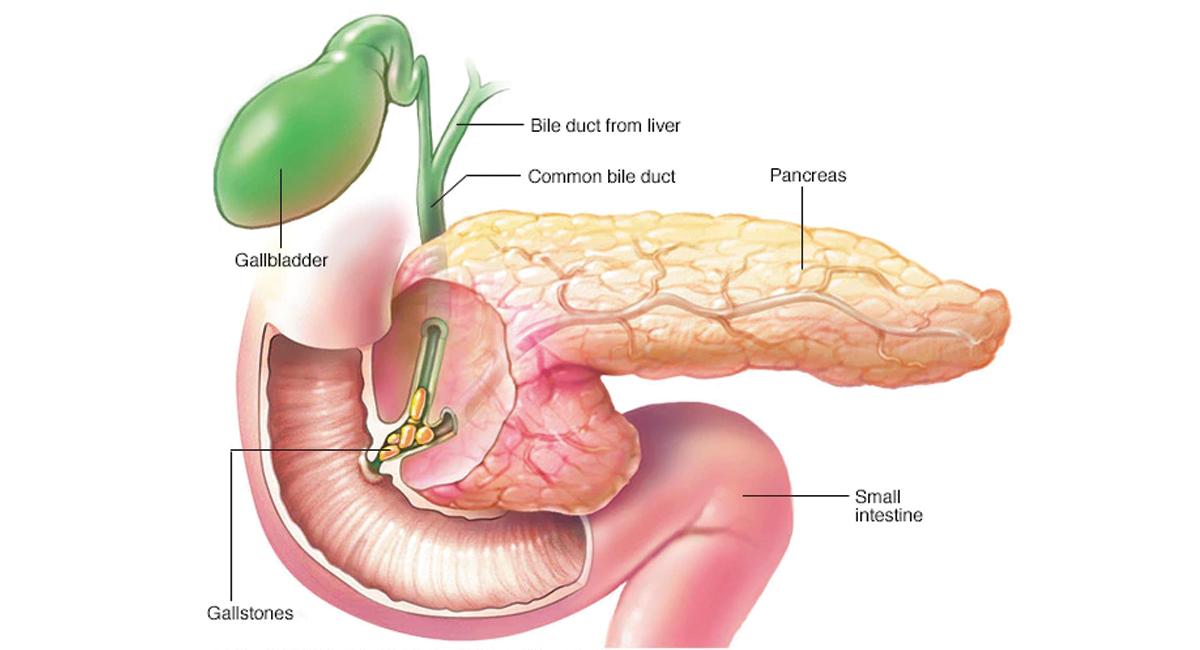
The pancreas is a large visceral organ present in your belly. It is located behind your stomach and primarily functions to release powerful digestive enzymes into your small intestine. This enzyme helps in the digestion of your food.
About Pancreatitis
Pancreatitis is the condition of an inflamed pancreas. There are two major functions of a pancreas: producing enzymes into the digestive system and producing hormones into the blood to regulate blood glucose levels. These hormones regulate the way your body processes glucose.
Pancreatitis can occur in an acute or chronic form. If it is sudden and lasts for a few days, it is known as acute pancreatitis. And, if it occurs over several years, it is known as chronic pancreatitis.
The severity may also vary. If it is a mild form, it can go away on its own, while the severe form can cause life-threatening complications.
What Causes Pancreatitis?
One of the most common causes of chronic pancreatitis is recurrent acute pancreatitis. It damages the pancreas forming scar tissues and causing a loss of function. This shows systemic malfunctions like diabetes and difficulty indigestion.
Following conditions usually lead to pancreatitis, while sometimes the cause may not be found:
- ● Alcoholism
- ● Cystic fibrosis
- ● Infection
- ● Gallstones
- ● Obesity
- ● Pancreatic cancer
- ● Certain medications
- ● Abdominal injury
- ● High triglyceride levels in the blood (hypertriglyceridemia)
- ● Abdominal surgery
- ● High calcium levels in the blood (hypercalcemia) caused by an overactive parathyroid gland (hyperparathyroidism).
- ● A procedure used to treat gallstones known as Endoscopic retrograde cholangiopancreatography (ERCP)
What are the Symptoms?
- ● Fever
- ● Nausea
- ● Vomiting
- ● Upper abdominal pain
- ● Tenderness when touching the abdomen.
- ● Abdominal pain radiating to your back.
- ● Rapid pulse
- ● Abdominal pain worsens after eating.
Chronic pancreatitis may cause the following symptoms:
- ● Unintentional weight loss.
- ● Pain in the upper abdomen.
- ● Steatorrhea or smelly stool.
How to diagnose?
- ● Computerized tomography scan to assess the extent of pancreatic inflammation and look for gallstones. It is usually done along with ultrasound imaging with the same intention. Endoscopic ultrasound is also done to assess any blockages in the pancreatic duct or the bile duct. MRI is also an investigation of choice.
- ● Blood tests to evaluate the levels of pancreatic enzymes. An elevated level is indicative.
- ● In chronic pancreatitis, a stool test is recommended to measure levels of fat in the stool. This could suggest your digestive system isn’t absorbing nutrients adequately due to impaired pancreatic functions.
Treatment of pancreatitis
In case you still develop pain in your abdomen after eating food, a feeding tube might be placed to help you get enough nutrition. Pain medications might also be given for severe pancreatitis pain.
Once you are stable, your doctor will move forward to identify the cause of your pancreatitis and take the necessary steps to treat it. The several treatments that are commonly done for pancreatitis are:
- ● Endoscopic retrograde cholangiopancreatography (ERCP) – It is a procedure to remove the bile duct obstruction. A tube with an inbuilt camera is inserted down the throat, and the procedure is followed.
- ● Cholecystectomy, or the surgery for removal of gallbladder stones, is performed.
- ● A pancreatic surgery might also be needed to remove excess fluid from the organ or, if needed, pancreatic tissues.
- ● If the cause is excessive drinking, this is treated with alcohol de-addiction programs. If you do not reduce or stop alcohol intake, your pancreatitis will become worse.
- ● Pain medications are generally given along with alternative therapy in chronic pancreatitis. If needed, surgery can be performed to block the nerve causing pain.
- ● You might be given pancreatic enzymes to be taken with each meal. This will suffice the lack of production.
- ● A low-fat meal diet will be given to you by your dietitian. Follow it to avoid further complications and develop pain in the abdomen again.
FAQ's
When to see a Doctor?
What are the Lifestyle Changes that are Needed?
Can Alternative Therapy Help in Treating Pancreatitis?
What Puts me at a Greater Risk of Developing Pancreatitis?
Is there a Change in Bowel Movement Due to Pancreatitis?
Need Help?
For any Information about our Locations, Doctors or Treatments.


