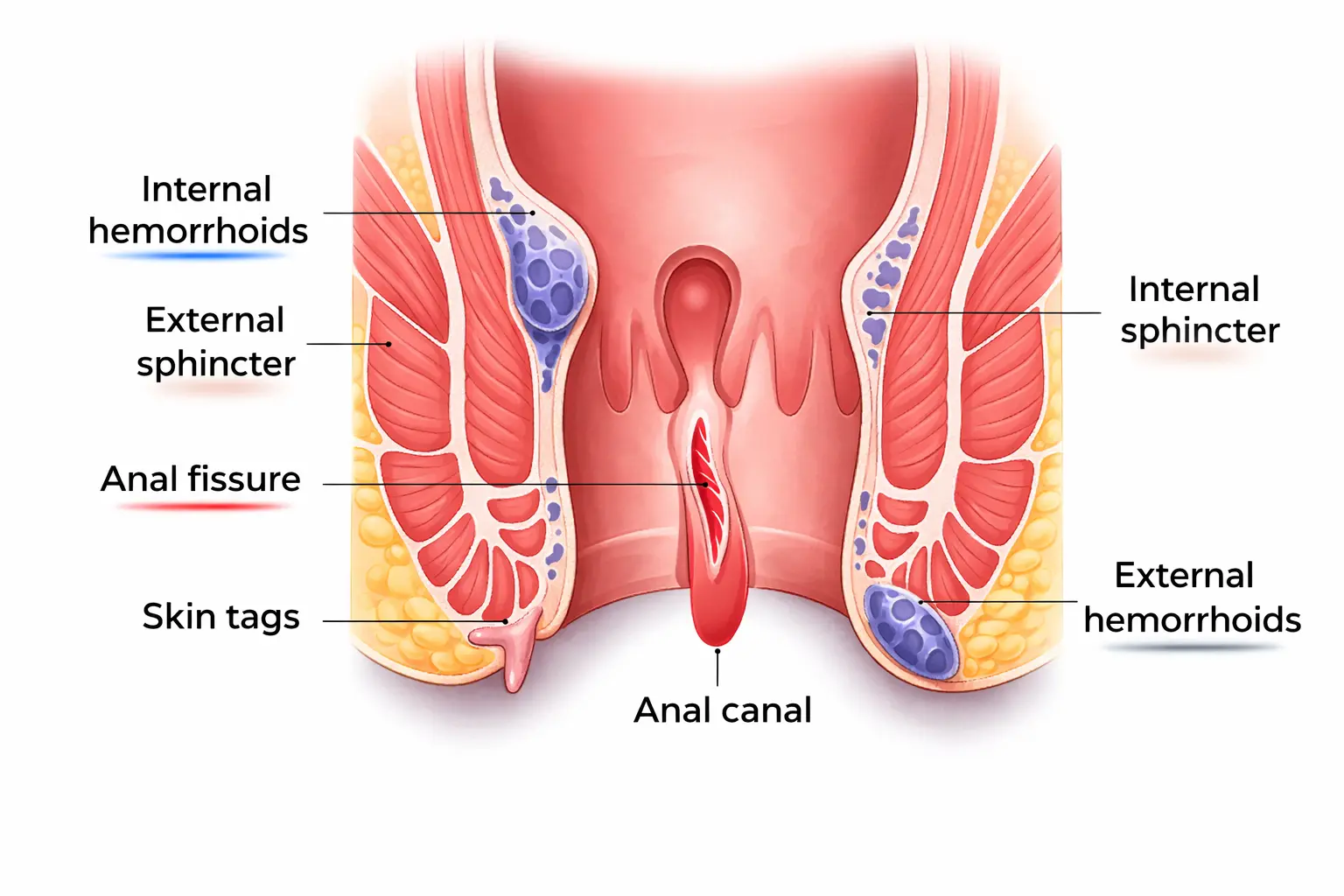
Anal fissures are a very common condition where there are superficial tears formed in the
skin which lines the anal opening. Since they form primarily due to intense straining when
passing bowels, they can develop irrespective of age or gender. However, due to their
superficial nature, they can also be easily cured. While home remedies do prove beneficial
for treating fissures, doctor recommended treatment strategy works best for permanent
relief, especially in case of recurring fissures. Read on till the end of this article for all the
must-know information about anal fissure treatment and who can help you during this
sensitive time.
What do you call a doctor who specialises in Fissures?
A doctor who gives specialised care for anal fissures is called a colorectal specialist or a
colorectal surgeon. Many people also colloquially use the term proctologist interchangeably.
It is common to think that a gastroenterologist can treat anal related conditions such as
piles, fissures, or fistulas. While this holds true, their scope of treatment is limited to
preventive care, and general non-interventional treatments to reduce the symptoms of
colorectal or anal related conditions.
A colorectal specialist is a doctor who has studied more in-depth about the colon, rectum,
and the anal regions of the human body. They obtain the necessary certifications to treat,
and perform non-invasive and invasive interventions to heal conditions related to these
parts. Thus, for effective and permanent relief from fissures, it is best to visit a colorectal
specialist or surgeon.
Can the same doctor treat fissures, and piles/hemorrhoids?
Yes! Simply put, piles are swollen veins in the rectum and anus. They are equally or more
common than fissures. Since a colorectal surgeon specialises in treating all conditions
related to the colon, rectum, and anal regions, the same doctor who treats fissures can also
treat piles. Although both the conditions may cause similar symptoms, they differ in how
they manifest physically, and how they need to be treated. Thus, for any colorectal or anal
conditions, it is best to visit a good colorectal specialist—a targeted treatment is far more
effective and quicker than generalised/preventative treatments.
What foods trigger anal fissures?
matter. According to studies, approximately 60% of the people suffering from chronic
constipation is due to dietary habits which do not support the formation of soft stools.
types which cause hard stools and reducing their intake immensely helps in decreasing
formation of anal fissures.
Below are some commonly heard foods which are the major causal factors of anal fissures.
content remaining in them. This means, once they get digested, they cannot absorb
water and their waste form also remains hard. Foods like fries, samosas, chips, all the
traditional Indian snacks fall in this category. Eating them consistently and in large
quantities is one of the major reasons why many people nowadays are experiencing
constipation.
material stage itself. This makes the final food also very low to absorb water or form
soft stools. Examples of processed foods include doughnuts, pizzas, white bread,
cakes, and biscuits. All these food types use ultra refined wheat flour (maida) and
huge amounts of sugar in their recipes, making them unfit to eat regularly.
chillies, pickles, hot sauces often cause burning sensation during bowel movements.
When this occurs frequently, it irritates the delicate mucosal lining of the anal canal
leading to cuts.
red meat cause constipation leading to anal fissures.
candidates which not normally known.
the body. These food types are tortilla or corn chips, popcorn, and nuts in large
quantities. While they are not well-known for causing constipation, their rough
texture irritates the delicate anal lining even if the stools are soft, causing minor tears
and cuts.
some fruits high in their acidic nature like oranges, lemons, grapefruits, and lime can
cause irritation to the lining by increasing the burning sensation. Limit their intake, or
choose alternatives like apples and pears which are delicate to the anal lining to
reduce fissure symptoms.
amounts, can intensify pain and burning when passing stools especially if the anal
area is already inflamed due to piles or other infections.
which can pass through the digestive tract intact. These seeds can increase irritation
and worsen pain if they get caught in the tiny tears of the existing fissures. Choose to
eat small quantities of these berries and more of blueberries which contain more
pulp than seeds.
are dense in fibre content. But many a time, they are either not accompanied with
equal hydration or consumed in too much quantities which makes it hard for the
digestive system to process them. Both these reasons can result in hard stools, and
fissures.
when consumed in exceedingly high quantities in a single day. Ensure not to avoid these
fruits or nuts as they are very high in their nutritional content. Best way to consume these
would be to eat them in moderate quantities, and pair them with ample hydration to
experience maximum benefit of nutrition and gut health.
How to treat Fissures in toddlers?
is one of the major causes of anal fissure formations. Hard bowels can be formed even in
toddlers due to low water and fibre intake. The delicate skin of a toddler makes it even
easier for tears and cracks to occur even under mild strain. However, treating anal fissures in
toddlers is focused more on home remedies rather than medical interventions. Home
remedies work to give quick relief as children have a quicker recovery time compared to
adults. Here are some easy steps to cure your toddler’s painful symptoms at home.
warm water is the most effective way to relax the anal sphincter muscle and increase blood
flow to the tear. Have your toddler sit in a clean tub with warm water 10–15 minutes for
thrice daily.
helps in faster healing. You can use
Coconut oil after drying the area gently. It acts as a natural antimicrobial and a
lubricant for the next stool.
Rash Creams: use a thick zinc-oxide cream (like diaper rash cream) to protect the
tear from being irritated by urine or stool.
Wiping: Use fragrance free wet wipes or a gentle spray of water rather than dry
tissue paper which can worsen the burning sensation.
pebble like stools keeps the fissures open and will not allow healing.
The “P” Fruits: Focus on Pears, Papaya, Prunes, and Peaches. These are natural
laxatives for kids.
Hydration: Ensure they are drinking plenty of water. Tender coconut water and
buttermilk (chaas) are excellent for keeping them hydrated.
important step. Pain often makes them afraid to pass stools again. When the stools back up
in the rectum, they become harder and more difficult to pass, in turn adding more pain
during bowel movements.
How do you permanently heal anal fissures?
Many people feel the pain of fissures at some point. However, when fissures recur
repeatedly, there is not enough time for the skin to heal. This is when a fissure becomes
chronic. In chronic fissures, the open skin causes constant pain, which makes the muscle
spasm. This spasm restricts blood flow to the tear, and without blood, the skin cannot heal.
Thus, to recover from the fissure completely, it is important to break this cycle of pain-blood
flow restriction.
Apart from the general home remedies like using sitz bath, increasing fibre and water intake,
and using stool bulking agents, a colorectal specialist will also recommend simple
procedures which can provide quick but permanent relief. These procedures will be strongly
advised specially when the fissures do not heal even after a month of following home
remedies.
weeks, your colorectal doctor may move to prescription ointments that chemically
relax the muscle to allow blood flow. Some examples are nitroglycerin (GTN)
ointment which increases nitric oxide to relax the muscle and boost blood flow, and
calcium channel blockers (Diltiazem/Nifedipine).
sphincter. It works by paralyzing the muscle for 2–3 months. This forced relaxation
allows the fissure to heal completely without the spasms.
LIS Surgery: A procedure called Lateral Internal Sphincterotomy (LIS) is considered
the most permanent cure for chronic fissures that don’t respond to other treatments.
Here, a surgeon makes a small cut in the internal sphincter muscle. This reduces its
resting tension. It has a success rate of over 95%, and most patients feel immediate
relief from pain within 24 hours.
and other habits which cause hard stools.
How risky is fissure surgery:
Patients also report a very quick recovery time from the sharp pain generally felt otherwise.
Thus, when done by an experienced colorectal surgeon, the benefits and healing time far
outweigh the risk significantly. However, there may be certain localised risks associated with
LIS like
Minor gas incontinence: About 5% to 10% of patients may have temporary difficulty
controlling gas.
Major Incontinence: This is very rare—less than 1%, when performed by an
experienced proctologist or colorectal surgeon.
Recovery: For the vast majority, this lack of control resolves on its own within a few
weeks as the area heals.
condition, and is extremely common. Dietary adjustments and lifestyle changes are the key
for fissure recovery; however, recurring fissures require personalised treatments in the
caring hands of a colorectal specialist. Remember, achieving permanent relief is possible
when you choose expertise over temporary fixes. At Smiles Gastroenterology Centre,
Bangalore, you can access world-class coloproctology, combining state-of-the-art technology
with care to ensure you can return to your daily life with smile and confidence.
Dr. Pavithra A is a Senior Colorectal Physician at Smiles Institute of Gastroenterology with over 14 years of clinical experience. Specializing in conditions like piles, fissures, and fistulas, she is particularly recognized for her expertise in treating colorectal issues in women and during pregnancy. Based in Bangalore, Dr. Pavithra is known for her empathetic approach and commitment to providing ethical, patient-centric care for complex digestive and anorectal disorders.